If you have recently been diagnosed with a meniscus tear, you are likely navigating a sea of medical terms, surgical options, and recovery timelines. As an Orthopaedic Surgeon in Delhi, I often see patients who are eager for a “quick fix” so they can return to the gym or the field. However, when it comes to long-term mobility, the goal shouldn’t just be speed—it should be preservation.
Choosing knee preservation surgery, specifically a meniscus repair, is an investment in your future. But here is the catch: unlike a simple “trimming” of the cartilage, a meniscus repair recovery is a marathon, not a sprint. Understanding the biology of how your knee heals is the first step toward a successful outcome.
Preservation vs. Removal: The Biological Choice
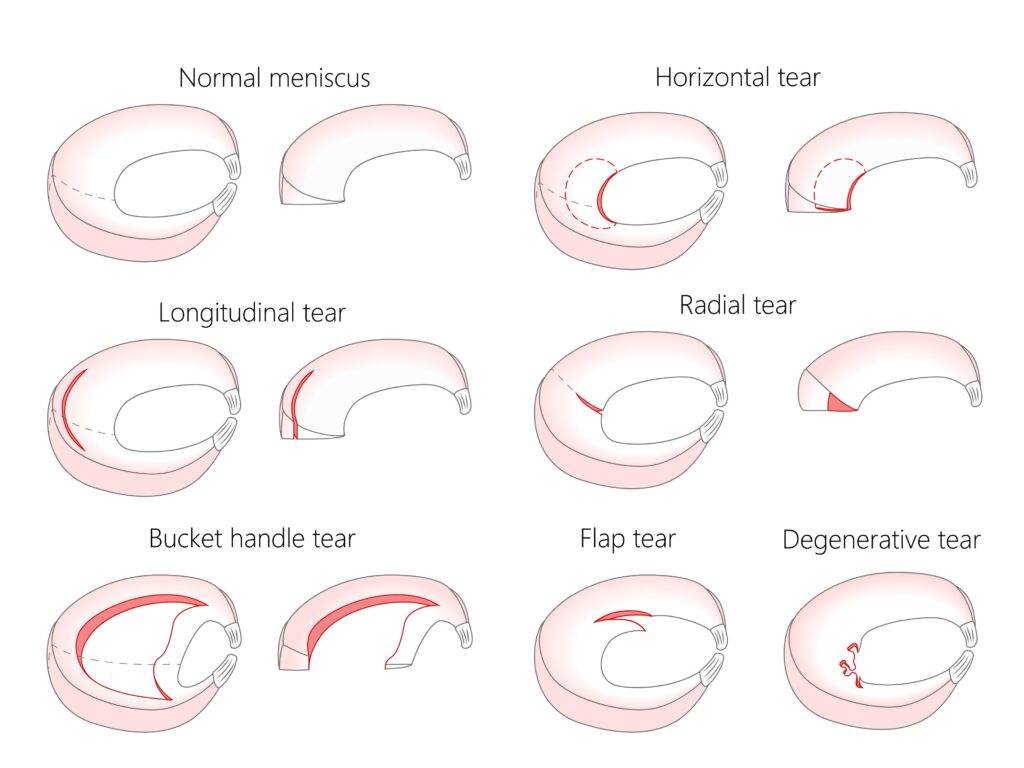
The meniscus is a C-shaped piece of tough, fibrous cartilage that acts as a shock absorber between your thighbone and shinbone. For years, the standard treatment was a meniscectomy—simply cutting out the torn portion. While this allows for a very rapid return to activity, it often leads to the early onset of arthritis because the knee has lost its natural cushioning.
Modern sports medicine now prioritizes knee preservation surgery. By suturing the meniscus back together, we save the shock absorber. However, because the meniscus has a limited blood supply, particularly in the “white-white” zone (the inner part of the meniscus), the healing process is delicate. We aren’t just fixing a mechanical break; we are waiting for the body to perform a biological miracle.
The “Healing First, Strength Later” Philosophy
The most common mistake patients make during their meniscus repair recovery is rushing into strengthening exercises. I always tell my patients: “We don’t build a house on wet concrete.”
In the first few weeks following surgery, your body is busy laying down new collagen fibers. This tissue is incredibly fragile. If you put too much load on the knee or bend it too deeply, you risk “cheese-wiring” the stitches through the soft cartilage. This is why the initial phase of recovery is about protection, not performance.
Phase 1: The Protection Period (Weeks 0–6)
During this window, your primary job is to be a “good healer,” not a “good athlete.” You will likely be:
- Using Crutches: To control the weight-bearing load on the healing tissue.
- Wearing a Brace: To limit the range of motion and prevent accidental twisting.
- Monitoring Swelling: Effusion (fluid in the joint) is the body’s way of saying it’s being pushed too hard.
The Checklist for a Successful Recovery
To ensure your knee preservation surgery is a success, there are non-negotiable precautions you must follow. As an Orthopaedic Surgeon in Delhi, I’ve observed that patients who respect these boundaries have significantly higher success rates.
- Avoid Deep Squats: Deep flexion puts immense pressure on the posterior horn of the meniscus, where many repairs are located.
- No Twisting: The meniscus is most vulnerable to rotational forces. Avoid pivoting on your leg.
- Patience with the Gym: It may feel like your quads are shrinking, and they might be. But it is much easier to rebuild a muscle than it is to re-repair a failed meniscus.
Why Biology Dictates the Timeline
Many people ask, “Why does a repair take six months when a trim takes six weeks?” The answer lies in vascularity. The outer rim of the meniscus (the red zone) has a decent blood supply, but the further inward the tear goes, the harder it is for the body to deliver the nutrients needed for repair.
During your meniscus repair recovery, we often use biological adjuncts like PRP (Platelet-Rich Plasma) to kickstart this process, but even with modern technology, we cannot force biology to move faster than it is designed to.
Long-term Benefits: The Return to Sport
The ultimate goal of any orthopaedic surgeon in Delhi is to get you back to the life you love. While the recovery for a repair is longer, the long-term results are far superior for athletes. By keeping your meniscus, you maintain the stability of your knee and protect your ACL and other ligaments from overcompensation.
When we finally clear you for “strength” after the “healing” phase, we do so with the confidence that the foundation is solid. You’ll work with physical therapists to regain your proprioception (balance) and power, gradually transitioning from walking to jogging, and eventually back to cutting and jumping.
Conclusion: Trusting the Process
A meniscus tear is a fork in the road. You can choose the short path (removal), which might get you back to work in two weeks but could lead to a knee replacement in twenty years. Or, you can choose the long path (repair), which requires six months of discipline but preserves your joint for a lifetime.
If you are looking for an orthopaedic surgeon in Delhi who specializes in these complex repairs, remember that the surgery is only 50% of the battle. The other 50% happens in your living room, on your crutches, and in your mind as you stay patient.
Respect the biology, trust the timeline, and remember: Healing First, Strength Later.
